Primary health care (PHC) is a critical aspect of health care delivery in Tennessee and around the world. Nevertheless, despite efforts made in recent years to improve PHC, there are still several challenges that affect the effectiveness of PHC in under-served and under-resourced communities in Tennessee and sub-Saharan Africa (SSA).
The America’s Health Rankings 2022 report, Tennessee is ranked at 44th among states for health outcomes placing Tennessee in the top 10 of the least healthy states in the United States.
In the same way, SSA health care systems are among the lowest in the world and only fewer than 50% of its population have access to health facilities. While the US is a high-income country unlike SSA, we still face the same primary health care challenges and many people living in rural settings and hard-to-reach areas are the populations particularly impacted due to limited access, limited resources, poor health outcomes, and limited public health education.
Hear more Tennessee Voices: Get the weekly opinion newsletter for insightful and thought provoking columns.
Featured letters by Muna Muday: How to make 2022 the last year of COVID-19
Women from minorities and rural areas suffer the most
Lack of access and unstable health systems are driving the problems to health care delivery, and it significantly exacerbates the shortage of health care facilities, health care workers, and inadequate transportation infrastructure.
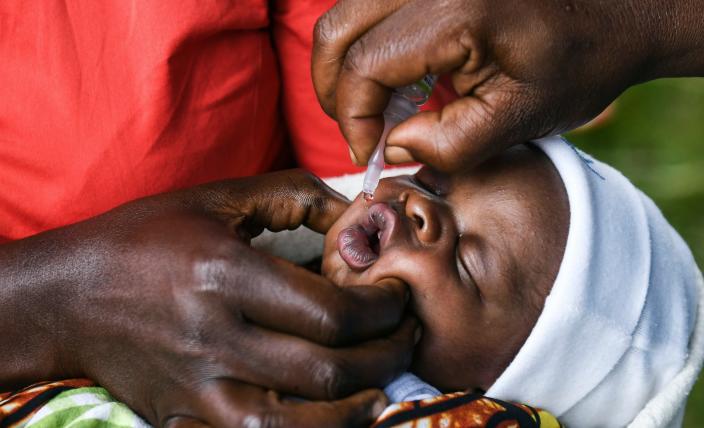
Consequently, with all the barriers existing in our PHC systems, it is very complicated to provide high-quality care to patients especially vulnerable individuals like pregnant women.
Tennessee currently accounts for the highest maternal mortality rate (MMR) in the United States almost similar to a developing country.
In 2020, Tennessee had 58.5 maternal deaths per 100,000 live births compared to SSA where 70% of the world maternal deaths occurred with a ratio of 533 maternal deaths per 100,000 live births.
Unfortunately, women from the minority and rural communities disproportionately suffer the most. Even though Tennessee is not a developing state, geographic and socioeconomic challenges have caused a lot of closure of many rural hospitals nationwide leaving many pregnant women and others without access to primary healthcare.
Likewise, PHC in Africa is rarely equipped to be the foundation of the healthcare system and is often used by patients seeking hospital services. Also, the 47 countries of sub-Saharan Africa have a critical shortage of frontline healthcare workers. There are two doctors and 11 nurses/midwifery personnel per 10,000 population, compared to 62 primary care providers (PCPs) per 100,000 persons in Tennessee.
Sign up for the Latino Tennessee Voices newsletter:Read compelling stories for and with the Latino community in Tennessee.
Sign up for the Black Tennessee Voices newsletter:Read compelling columns by Black writers from across Tennessee.
The closures of rural hospitals pose a health threat
Although the battling of provider shortages has increased globally with the COVID-19 both in Tennessee and SSA the differences vary significantly. In SSA, doctors are rarely seen in primary care or in rural or remote areas and the health workers who form the main primary care workforce in SSA have limited training, limited range of resources, such as medications and supplies, and the few resources available are often concentrated in prestigious central referral hospitals.

In addition, governance systems are weak with a lack of supportive supervision and managerial leadership. SSA has 25% of the global disease burden, but only 3% of the world’s health workers and less than 1% of the world’s health expenditure. Tennessee spent $10.2 billion in health expenditure in 2019. Nonetheless, there is also a relative shortage of physicians in rural Tennessee communities as well because doctors who are highly specialized are less likely to settle in a rural area and systems are growing slowly in rural areas and their doctors may be of little use to the working poor who have neither Medicaid nor conventional health insurance.
Undoubtedly, addressing strong PHC plays a key role in the provision of and access to vital health care services for hard-to-reach populations in Tennessee, SSA, and around the globe. As I passionately wrote this guest essay, I am currently the director of programs at a Tennessee-based global health organization called The Addis Clinic, where I am part of a team working to improve access to primary health care in East Africa through the delivery of digital health interventions and telemedicine services in order to strengthen existing health systems and build health worker capacity.
Digital healthcare is one of the simplest ways to also find solutions for health disparities and promote health equity. Through digital health innovations we can be both impactful and useful in under-served and under-resourced communities and fight future pandemics in Tennessee and around the world.
Muna Muday, MPH, is director of programs at The Addis Clinic.
This article originally appeared on Nashville Tennessean: Tennessee health care faces similar challenges to sub-Saharan Africa

